What do swollen turbinates look like
If you’ve never heard of turbinates before then you’re not the only one! As long as they’re working well then the subject is unlikely to ever come up; they are also not something that your regular doctor (GP) is able to review – finding out there’s a problem first requires a referral to an Ears Nose Throat (ENT) specialist because of the symptoms you are experiencing.
Your turbinates can have a surprisingly large impact on your quality of sleep; this is especially true in young children and the problems are even more exacerbated if they also have troubles with their ears, adenoids, and tonsils.
What are turbinates?
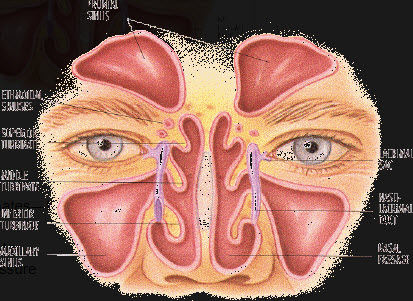
Turbinates are bony structures (covered in moist tissue called the nasal mucous membrane). Inside your nose there are three sets of turbinates: upper (superior), the middle, and the lower (inferior).

Lateral Nasal Airway: Turbinates, Adenoids, Eustachian Tube Opening
Why do we need turbinates? What do turbinates do?
The turbinates have several important functions:
- Help warm and moisturize air as it flows through the nose.
- Protect the openings into your paranasal sinuses.
- Help create airflow through your nose (important for your sense of smell!).
- Trap micro-organisms (like viruses) and pollutants (like pollen).
- Help the voice to resonate (i.e. they affect how we sound).
- Produce mucous to help clean out the nose and assist the cilia in their work.
- Help to regulate pressure in the sinuses.
- Help the nose and sinus cavities to drain.
- The turbinates play an important mechanical function when we sleep. When you sleep on the right side, with the right turbinate down, over time the right turbinate fills up with fluid and expands so that it pushes against the septum; this makes you turn on the left side until that side fills up and turns you again. If the turbinates are not functioning correctly then you may wake up feeling cramped and sore with achey muscles.
Feeling the pressure? Healthy turbinates help regulate pressure and drainage of the sinus cavities.
What causes turbinates to swell?
One of the most common causes of swollen turbinates (turbinate hypertrophy) are airborne allergies (allergic rhinitis) such as grass or weed pollen, birch tree pollen, or dust mites.
Other causes can include repeat upper respiratory infections, hormones, drugs, medication (i.e. as a complication from long-term nasal spray use).

Healthy inferior turbinate – you can see quite clearly that there is a tunnel for air to flow freely past the turbinates.

Swollen turbinates – you can see how they have swollen and are bulging out across the airway to the nasal septum.
What are the possible side effects of swollen turbinates?
- Stuffy nose
- Headache
- Facial Pain
- Pressure (often in forehead). In young children this may result in behavioural issues, trouble concentrating, or head banging.
- Nasal drip
- Loss of Sense of Taste and/or Smell
- Mouth breathing, noisy breathing, and/or snoring. This is especially problematic if adenoids and/or tonsils are also swollen and obstructive sleep apnea develops.
- Fatigue. Children might seem like they’re getting enough hours of sleep but in reality the quality of sleep is poor because their body is struggling to get enough oxygen through the night. It’s a bit like starting each day on a half tank of gas.
- Sore, cramped, achey muscles in the morning. Healthy turbinates play an important mechanical function when we sleep; they are key to helping us unconsciously change which side we are sleeping on through the night.
- Developmental delays. Sleep is critical for young children. During those early years, they are rapidly growing and learning. They need sleep to focus during the day; to have time for their brain to make connections between all the things they have learned or experienced; and their brain releases a growth hormone while they sleep. Poor sleep, fatigue and pain/discomfort, trouble hearing: these can make it harder for them to stay on track.
- Behavioural difficulties. Poor sleep, fatigue and pain/discomfort, trouble hearing: these can result in daily misery that children don’t know how to express.
Why do turbinates need surgery?
An Ears Nose Throat (ENT) specialist will be able to examine the interior of the nose quickly and painlessly during outpatient appointments; they may also opt for imaging scans such as x-ray or CT.
It is likely that they will suggest trying non-invasive means initially to see if this reduces the swelling, This is likely to involve a steroidal nasal spray and anti-histamine medication (in the case of allergic rhinitis). They may also recommend additional saline spray / drops to help keep the nose irrigated, or using a humidifier.
If these options do not work an symptoms have not been alleviated then they are likely to recommend surgery. Note: it is important that turbinates are reduced (not removed) and they will slowly regrow; in order for them not to become swollen again, any other underlying issues must still be addressed.
What does turbinate reduction surgery (turbinoplasty) involve?
Turbinates perform highly important functions and removing them entirely can cause a raft of new issues; surgeons will normally opt to reduce the turbinates. There are different methods that can be used; some remove tissue and others aim to shrink them through other means.
A procedure called submucosal resection is a common technique used to treat enlarged turbinates. With this procedure, the lining of the turbinate is left intact, but the “stuffing” from the inside of the turbinate is removed. As the turbinate heals, it will be much smaller than before surgery. Sometimes, this resection can be performed with a device called a microdebrider. This device allows the surgeon to remove the “stuffing” through a small opening in the turbinate. In some instances, more of the turbinate is removed.
Some of these methods shrink the turbinates without removing the turbinate bone or tissue. These methods include cauterization, coblation, and radiofrequency reduction. In each of these methods, a portion of the turbinate is heated up with a special device. Over time, scar tissue forms in the heated portion of turbinate, causing the turbinate to shrink in size.
Turbinoplasty is generally an outpatient procedure performed under general anaesthetic and patients can go home the same day.
Want to find out more about surgery or risks? The American Rhinologic Society has useful information.
What happens after surgery?
You can expect to have pain, fatigue, nasal stuffiness, and a clear fluid nasal discharge for several days after surgery. If this was the only surgery being performed then pain is generally mild and typically well controlled with pain medications. A saline spray and/or steroidal nasal spray are likely to be recommended to use for several weeks after the surgery.
Swelling as a result of the procedure means that there may still be snoring for a week or two after the surgery, as well as a general feeling of stuffiness. The fluid discharge will generally begin to improve and crust after the first week.
Patients may be off school or work for a week and are recommended to avoid strenuous activity for two to three weeks afterwards.