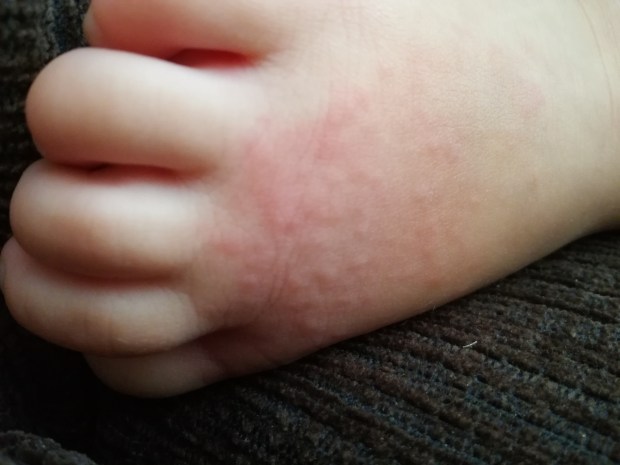
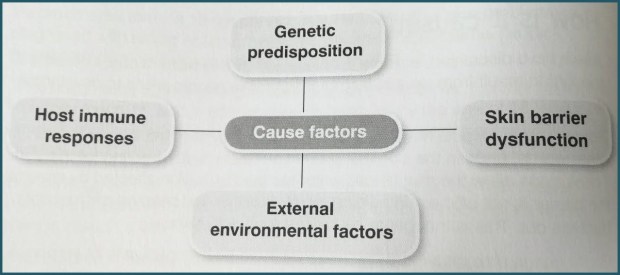
Eczema – the painful cycle of inflammation
Eczema cannot be cured. It can be treated and managed; key to this is caring for skin and managing the cycle of inflammation. Ensure that you discuss treatment with a medical professional; it’s also a good idea to ask what they can prescribe (as this may be free or discounted) as this often includes soap replacements and moisturisers as well as treatment creams.
Moisturise
It’s important to keep skin supple and moisturised. It’s a good idea to bathe every day (as the water will help to hydrate skin) and avoid soaps and other products that will have a drying effect. I’ve heard some people find goats milk soap to be gentler than normal soap and some emollient lotions can be used as soap replacements (though you may find they do better in a shower than a bath as I’ve found they can be kind of gluggy in bath water).
It’s a good idea to moisturise every day even when eczema isn’t flared up. Be careful when selecting moisturisers as general ones often contain alcohol that can still have a drying effect. It’s a good idea to discuss options with your doctor or pharmacist, and to look for ones endorsed by an eczema association.
Also, try different ones. You might find that some work better for you than others or that you prefer the smell or texture of some over others. I have a sorbitol/glycerin cream from the doctor which is ‘fragrance free’ but which I personally think smells so bad, v.s. one from Curash which I don’t think smells at all.
First: Emollients
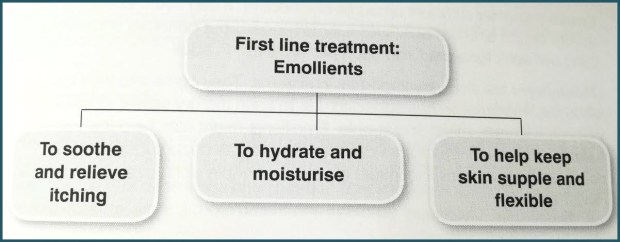
Emollients are basically moisturisers that are essential for increasing skin hydration and mimicking the barrier effect of the surface lipids the skin is lacking.
These should be used at least once a day at a different time to when corticosteroids are applied (as they will dilute these and prevent them from being as effective). It’s most effective to apply emollients after a warm bath or shower while skin is still damp.
Types of Emollients
From most effective to least effective.
- Ointment – This provides a ‘lock-in’ protective layer. It can leave a greasy film so is often preferred at night (over day).
- Cream – Thinner and easier to apply. It is less effective than ointment and will need to be applied more often.
- Lotion – Has a runny consistency and is less effective again than cream.
Generally, the rougher and drier the skin is, the thicker the emollient that is required. So a lotion may be suitable when when skin is good but cream, and then ointment, as it gets worse.
Emollients are important as part of a daily routine and will help to soothe skin during a flare-up. They will not treat the inflammation and it is important that a treatment cream is also used.
Second: Corticosteroids
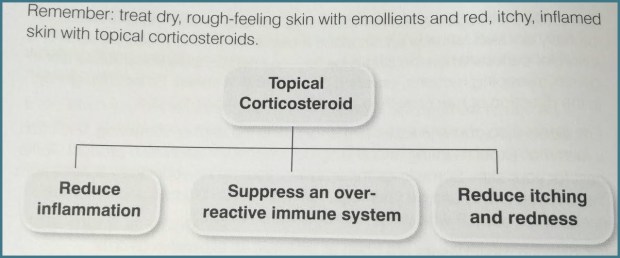
Topical corticosteroids (like hydrocortisone) actually treat the inflammation and help to reduce itchiness. They help to reduce blood flow in the skin and suppress over-active infection-fighting white blood cells. They imitate the effects of cortisol hormones produced naturally in the adrenal glands.
Doctors may prescribe different strength corticosteroid creams for different parts of the body (i.e. a weaker one for the face, and a stronger one for feet or hands where skin is thicker).
Additional treatments
Depending on the severity of symptoms, doctors may also discuss additional treatment options such as wet wrap, or oral anti-histamines.
There is little research supporting the effectiveness of using oral antihistamines to treat eczema but they can provide relief; for instance, night time ones can temporarily ease inflammation and also cause drowsiness. Not only is scratching bad for the skin but chronic sleeplessness (due to lying in bed scratching) can cause a raft of flow-on troubles, especially for young children, so a night anti-histamine is something to consider discussing with your doctor.
Key source: “Eczema: The Essential Guide” by Sharon Dempsey